“The truth will set you free, but first it will make you uncomfortable.” – Gloria Steinem
In today’s hyperconnected world, information about fertility is everywhere and yet, paradoxically, clarity is often nowhere to be found. Social media reels, whispered family advice, half-read Google searches, and outdated cultural beliefs have created a dense fog around one of the most fundamental aspects of women’s health.
For many young women, fertility is either shrouded in premature panic or wrapped in dangerous complacency. Some are told they have “plenty of time,” while others are pressured into urgency before they even understand their own bodies. Between these extremes lies a quieter truth: fertility is deeply individual, biologically nuanced, and socially influenced.
In our previous article, Teen Minds Under Pressure: How Girls Can Stay Strong, we explored how mental wellbeing shapes a girl’s relationship with her body. Fertility awareness builds on that foundation. When women understand their reproductive health without fear or misinformation, they make decisions rooted in confidence rather than confusion.
This conversation is not about inducing anxiety. It is about replacing myths with medically grounded understanding, and empowering women to navigate their reproductive years with agency.
Because fertility is not just a biological event, it is a life journey influenced by health, timing, environment, and choice.
The Biology Behind Fertility: What Every Woman Should Truly Know
At its core, fertility is governed by a sophisticated orchestration of hormones, ovarian function, and reproductive timing. Each menstrual cycle represents a delicate hormonal symphony involving the brain, ovaries, and uterus.
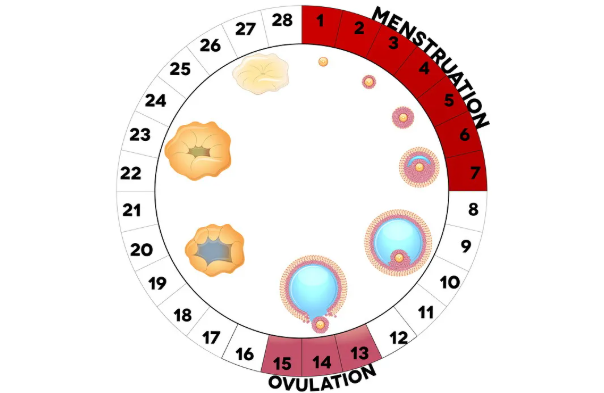
Ovulation, when an ovary releases an egg is the pivotal event. However, contrary to popular belief, ovulation does not occur on the same day for every woman, nor does every cycle look identical. Cycle length, hormonal patterns, and ovulatory consistency vary widely.
Female fertility is also age-sensitive. Women are born with a finite number of eggs, and both egg quantity and quality gradually decline over time. This is a biological reality, not a social judgment. Yet the rate of decline differs significantly among individuals.
Moreover, fertility is not solely a “woman’s issue.” Male factors contribute to a substantial proportion of infertility cases globally. Still, the cultural burden of blame disproportionately falls on women a disparity that must be challenged through education.
Understanding the biology does not mean predicting the future with certainty. Instead, it provides a compass for informed decision-making.
Myth One: “If Your Period Is Regular, Your Fertility Is Perfect”
One of the most pervasive misconceptions is that regular menstrual cycles automatically indicate optimal fertility. While cycle regularity often suggests ovulation is occurring, it does not guarantee that ovulation is consistent every month or that egg quality is unaffected.
Conditions such as mild hormonal imbalances, thyroid disorders, endometriosis, or early-stage polycystic ovary syndrome (PCOS) can exist even in women with seemingly regular cycles. Additionally, factors like stress, sleep disruption, and metabolic health can subtly influence reproductive function without immediately altering cycle timing.

The danger of this myth lies in false reassurance. Many women assume there is no need to understand their reproductive health more deeply until they encounter difficulty conceiving. By that point, valuable time may have passed.
The empowering alternative is proactive awareness. Tracking cycles, understanding ovulation patterns, and seeking medical guidance when irregular symptoms appear can provide earlier insight into reproductive health.
Regular periods are a helpful signal but not the full story.
Myth Two: “Fertility Only Declines After 35”
The age of 35 has become a cultural milestone often referred to sometimes dramatically as the fertility cliff. While it is true that fertility decline becomes more noticeable in the mid-30s, the biological process begins earlier and progresses gradually.
Egg quantity and quality begin to decrease in the late twenties for many women, though the pace varies widely. Importantly, this does not mean women in their early thirties cannot conceive naturally; many do. The danger lies in oversimplified messaging that either creates panic or fosters unrealistic reassurance.
Modern life trajectories like extended education, career building, financial plannings mean many women consider pregnancy later than previous generations. This makes accurate fertility literacy more important than ever.
The goal is not to rush life decisions. It is to ensure women are making them with clear biological awareness rather than comforting myths.
Myth Three: “Infertility Is Usually the Woman’s Fault”
This myth is not only scientifically incorrect but it is deeply harmful.
Global data from the World Health Organization (WHO) consistently shows that male factors contribute to infertility in a significant proportion of couples. In many cases, fertility challenges involve combined factors from both partners or remain unexplained.
Yet culturally, women often bear the emotional burden, social scrutiny, and self-blame. This imbalance can intensify psychological distress and delay appropriate evaluation of both partners.
Fertility is a shared biological equation. Any evaluation of conception difficulties must include both partners from the outset.
Shifting this narrative is not merely medically sound, it is socially just.
Modern Lifestyle and Fertility: The Invisible Influencers
Today’s fertility landscape is shaped not only by biology but also by environment and lifestyle. Chronic stress, ultra-processed diets, sedentary routines, sleep deprivation, smoking, alcohol misuse, and exposure to environmental pollutants can all influence reproductive health.
Metabolic conditions such as insulin resistance frequently discussed in our earlier PCOS article, also intersect with fertility outcomes. Even subtle hormonal disruptions can affect ovulatory patterns.
Importantly, this is not about perfectionism or blame. Many of these factors are embedded in modern living. The empowering message is that small, sustainable lifestyle shifts can meaningfully support reproductive health.
Balanced nutrition, regular physical activity, adequate sleep, and stress management are not quick fixes but they are powerful long-term allies.
When to Seek Help: Recognizing the Right Time
One of the most common sources of confusion is knowing when to consult a healthcare professional.
General medical guidance suggests that women under 35 who have been trying to conceive for 12 months without success should seek evaluation. For women over 35, that window shortens to six months. However, earlier consultation is wise if menstrual cycles are highly irregular, ovulation is uncertain, or known conditions like PCOS or endometriosis are present.
Seeking help is not an admission of failure. It is an act of proactive self-care and informed planning.
Fertility assessments today are far more sophisticated and accessible than in previous decades. Early conversations can provide reassurance, identify treatable issues, or simply offer a clearer reproductive roadmap.
Emotional Realities: Fertility and Mental Wellbeing

Fertility conversations often focus intensely on biology while overlooking emotional terrain. Yet uncertainty about reproductive health can provoke anxiety, self-doubt, and social pressure especially in cultures where motherhood expectations remain strong.
This connects directly to themes explored in Teen Minds Under Pressure, where we examined how early emotional resilience shapes later health experiences. Women who develop strong mental health support systems earlier in life often navigate fertility uncertainty with greater psychological steadiness.
Healthcare providers must increasingly adopt trauma-informed, emotionally sensitive fertility care. Information alone is not enough. Compassionate communication matters profoundly.
Women deserve clarity without fear and support without judgment.
From Awareness to Agency: Rewriting the Fertility Narrative
The future of women’s health depends on shifting fertility conversations from secrecy to science, from stigma to strategy, from pressure to personal choice.
Fertility literacy should begin early within age-appropriate reproductive education and continue through adulthood. It should be inclusive of diverse life paths, including women who choose not to pursue motherhood.
When women understand their bodies, they gain negotiating power over their timelines, healthcare decisions, and life planning.
Awareness is not about narrowing choices. It is about expanding informed freedom.
Understanding fertility is only half the equation. True reproductive empowerment requires both the knowledge of how conception occurs and the freedom to decide if and when it should. The journey toward reproductive justice is incomplete without equitable access to contraception, accurate education, and bodily autonomy. we move forward in this series, the next article will examine a crucial companion topic: Access to Contraceptives: Barriers & Rights.
- World Health Organization – Infertility Fact Sheet
https://www.who.int/news-room/fact-sheets/detail/infertility - Office on Women’s Health – Fertility and Infertility https://www.womenshealth.gov
- Centers for Disease Control and Prevention – Infertility Overview https://www.cdc.gov/reproductivehealth
- Resolve: The National Infertility Association https://resolve.org
