A quiet storm is unfolding in the bodies of young women across the world one that many people misread, frequently dismiss, and far too often diagnose late. It does not always announce itself dramatically. Sometimes it begins with irregular periods. Sometimes with stubborn acne, unexplained weight gain that refuses to yield despite sincere effort.
This storm has a name: Polycystic Ovary Syndrome (PCOS).
What makes PCOS particularly concerning today is not just its prevalence, but its increasing early onset among adolescents and young adults. Many girls spend years confused about what their bodies are trying to tell them. Healthcare providers often reassure them that “it’s just hormones” or tell them to simply “wait it out.” Meanwhile, the condition quietly progresses.
In our previous article, Stronger Futures Start with Better Reproductive Health Education, we emphasized that early knowledge equips young people to recognize warning signs in their own bodies. PCOS is precisely why that education matters. Because when awareness comes late, intervention often comes later.
As Maya Angelou once wrote:
“When you know better, you do better.”
In the context of PCOS, knowing earlier can change the entire trajectory of a young woman’s health.
Understanding PCOS: More Than Just Irregular Periods
PCOS is one of the most common hormonal disorders affecting women of reproductive age. Yet despite its prevalence, it remains widely misunderstood.
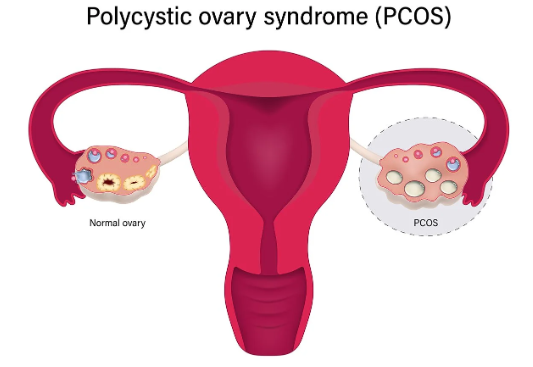
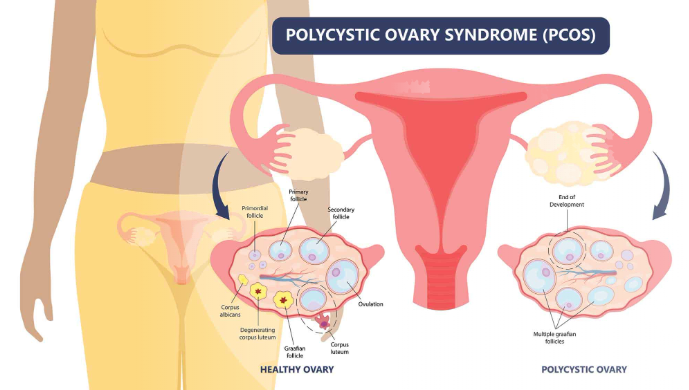
At its core, PCOS is a complex endocrine and metabolic condition. It typically involves hormonal imbalance, particularly elevated androgens (often called “male hormones”), irregular ovulation, and sometimes the presence of multiple small follicles in the ovaries visible on ultrasound.
However and this is crucial as PCOS is not just a reproductive issue. It is a whole-body condition that can affect metabolism, mental health, skin, hair growth, and long-term risks such as diabetes and cardiovascular disease.
For young women, the early signs often appear subtly. The body whispers long before it shouts.
Why PCOS Cases Are Rising Among Young Women
Healthcare providers across clinics and research settings now witness a conspicuous and somewhat unsettling pattern: PCOS diagnoses among adolescents and young adults continue to rise. No single cause drives this surge. Instead, a complex, interwoven web of biological vulnerability and modern lifestyle shifts fuels this growing trend.
Today’s young generation is growing up in an environment vastly different from that of previous decades. Sedentary academic routines, prolonged screen exposure, ultra-processed food consumption, chronic academic pressure, sleep deprivation, and rising insulin resistance are collectively reshaping metabolic health at an earlier age. These factors create a fertile ground for hormonal dysregulation, particularly in individuals who already carry a genetic predisposition.
However, there is another layer to this story one that offers cautious optimism. Improved awareness among healthcare providers and wider screening practices mean that cases previously overlooked are now being identified. What once remained hidden behind the label of “irregular teenage hormones” is increasingly being recognized as a diagnosable endocrine condition.
The World Health Organization has already acknowledged PCOS as a significant global women’s health concern, particularly in low- and middle-income settings where delayed diagnosis remains common. What is becoming unmistakably clear is that PCOS is no longer peripheral. It is emerging as a central public health priority.
Recognizing this rise early allows us to respond proactively rather than reactively, a shift that could redefine outcomes for an entire generation of young women.
The Early Clues Many Girls Miss
One of the most challenging aspects of PCOS in adolescence is its subtlety. The early signals rarely arrive dramatically. Instead, they appear as scattered, easily dismissed changes that blend into the already complex landscape of puberty.
Irregular menstrual cycles, for instance, are often considered “normal” in the first few years after menarche. While some variation is expected, persistently unpredictable cycles can be an early hormonal red flag. Unfortunately, many girls and sometimes even caregivers are reassured too quickly, allowing patterns to go untracked.
Persistent or severe acne is another frequently minimized clue. In many cases, it is treated purely as a dermatological inconvenience rather than explored as a possible endocrine signal. Similarly, unexplained weight gain or difficulty losing weight is often attributed solely to lifestyle habits, without deeper metabolic evaluation.
For some young women, increased facial or body hair growth becomes a silent source of embarrassment. Others notice thinning hair along the scalp and assume it is temporary stress-related shedding. Each symptom alone may seem minor. Together, however, they often form a coherent clinical pattern that deserves attention.
Early recognition does not mean catastrophizing normal puberty. It means cultivating body literacy, the ability to notice persistent patterns and seek timely guidance. When girls are empowered to observe rather than ignore their bodies, the entire trajectory of PCOS management can shift toward earlier, gentler intervention.
The Emotional Toll: PCOS Beyond the Physical
What remains profoundly under-acknowledged in many clinical conversations is that PCOS is not merely a hormonal condition, it is also an emotional experience. Adolescence and early adulthood are already seasons of intense self-formation. When visible physical changes emerge unpredictably, they can quietly erode confidence and body trust.

Young women navigating persistent acne, rapid weight fluctuations, or unwanted hair growth often report feeling alienated from their own reflection. Many describe a creeping frustration: doing “everything right” yet seeing their bodies behave unpredictably. Over time, confusion can morph into self-blame, and self-blame can deepen into shame.
Delayed diagnosis frequently compounds this distress. When symptoms are repeatedly dismissed as “just teenage changes,” young women may internalize the belief that their concerns are exaggerated or unimportant. This psychological invalidation can be as heavy as the physical symptoms themselves.
Emerging research consistently shows higher rates of anxiety, depressive symptoms, and body image distress among individuals living with PCOS. This connection is not coincidental. Hormonal fluctuations, metabolic stress, and social pressures intersect powerfully during adolescence.
This is precisely why our upcoming article, Mental Health in Teen Girls: Pressures, Body Image, and Support Systems, will explore this emotional dimension in depth. Because meaningful PCOS care must extend beyond lab reports, it must honor the whole person behind the hormones.
The Diagnosis Dilemma: Why PCOS Is Often Missed
Diagnosing PCOS during adolescence is a nuanced clinical challenge. Unlike many conditions that rely on a single definitive test, PCOS diagnosis depends on a constellation of findings are menstrual patterns, signs of androgen excess, biochemical markers, and sometimes ultrasound features.
The difficulty lies in the overlap between normal pubertal development and early PCOS features. Irregular cycles can be physiologically normal in the early post-menarche years. Acne is common in teenagers. Even mild hormonal fluctuations are part of typical maturation. Distinguishing what is transient from what is persistent requires clinical patience and careful longitudinal observation.
Unfortunately, this complexity often results in diagnostic delay. Many young women spend years moving between dermatology clinics, general practitioners, and gynecology visits before receiving a coherent explanation. During this window of uncertainty, metabolic risks may quietly progress.
Overdiagnosis is also a risk when criteria are applied too aggressively in adolescents. This makes balanced, evidence-based evaluation essential. What young women need most is neither dismissal nor premature labeling but thoughtful, informed monitoring.
Strengthening reproductive health literacy in schools, as discussed in our previous article, is one of the most powerful ways to shorten this diagnostic gap. When girls understand menstrual patterns and hormonal signals, they become active participants in early detection rather than passive recipients of delayed care.
Long-Term Health Risks: Why Early Action Matters
PCOS is often first recognized through visible symptoms, but its deeper significance lies in its long-term metabolic and reproductive implications. When left unaddressed, the condition can quietly influence health trajectories well into adulthood.
Insulin resistance is one of the most common underlying features of PCOS. Over time, this metabolic strain can increase the risk of developing type 2 diabetes. Lipid imbalances may elevate cardiovascular risk later in life. Chronic ovulatory dysfunction can create fertility challenges for some women when they eventually plan pregnancies. Sleep disturbances and mood disorders may also persist if the condition remains unmanaged.
Yet it is crucial to shift the narrative away from alarmism. PCOS is highly manageable, particularly when identified early. Many young women with timely support go on to experience regular cycles, improved metabolic health, and healthy pregnancies when desired.
The most powerful intervention is not panic, it is proactive, sustained care. Early screening, lifestyle alignment, appropriate medical guidance, and emotional support together can dramatically alter long-term outcomes.
When we intervene early, we do more than manage symptoms. We protect futures.
Lifestyle as Medicine: Small Changes, Powerful Impact
Among the most encouraging aspects of PCOS management is the profound responsiveness of the condition to supportive lifestyle shifts. While medical therapy plays an important role for many individuals, foundational metabolic care often begins with daily habits that stabilize hormonal rhythms.

Nutrition that supports steady blood sugar are rich in fiber, balanced proteins, and minimally processed foods can improve insulin sensitivity over time. Regular physical movement enhances metabolic flexibility and reduces inflammatory load. Consistent sleep patterns help regulate endocrine signaling. Stress-buffering practices such as mindfulness, yoga, or structured relaxation can further support hormonal balance.

However, it is essential to approach lifestyle care without blame or perfectionism. Young women do not need rigid, punishing routines. They need sustainable, compassionate structure. Small, consistent shifts often produce more durable results than extreme, short-lived changes.
Equally important is recognizing that responsibility cannot rest solely on individuals. Families, schools, food environments, and healthcare systems must make healthy choices accessible and realistic. When supportive ecosystems exist, lifestyle medicine becomes empowering rather than overwhelming.
The goal is not aesthetic transformation. The goal is metabolic resilience and hormonal harmony.
The Role of Schools and Families in Early Detection
Because PCOS often begins to surface during adolescence, the environments surrounding young girls play a pivotal role in early recognition. Schools and families are not merely observers, they are powerful enablers of timely awareness.
When reproductive health education is comprehensive, stigma-free, and scientifically grounded, girls become more attentive to menstrual patterns and bodily changes. They are more likely to track cycles, ask questions, and seek help early. Silence, by contrast, breeds delay.
Within families, open and non-judgmental conversations about periods, body changes, and emotional fluctuations create psychological safety. When parents respond with curiosity instead of discomfort, girls learn that their health concerns deserve attention.
School health programs can further normalize menstrual literacy by encouraging cycle tracking, hosting adolescent health sessions, and integrating hormonal health into life-skills education. Even simple awareness campaigns can shift cultural discomfort into informed dialogue.
Early detection rarely emerges from a single medical appointment. It grows out of an ecosystem of awareness, trust, and education. When that ecosystem strengthens, diagnostic delays shrink and young women step into care pathways sooner and with greater confidence.
From Silence to Strength: Rewriting the PCOS Narrative
For decades, PCOS has lived in the margins of public health discourse are often frequently misunderstood, sometimes minimized, and too often reduced solely to a fertility concern. That narrow framing has obscured the broader metabolic, emotional, and lifelong dimensions of the condition.
Today, however, the narrative is beginning to evolve. Young women are asking sharper questions. Digital health literacy is expanding. Clinicians are increasingly recognizing the need for adolescent-specific diagnostic sensitivity. Research momentum is growing.
Yet progress remains uneven, and complacency would be premature. PCOS awareness must move decisively into school curricula, primary healthcare conversations, community outreach programs, and digital health platforms. Screening guidelines for adolescents need continued refinement. Mental health integration within PCOS care pathways must become standard, not optional.
When knowledge expands, stigma contracts. When early screening improves, long-term risks decline. And when young women understand their bodies, the story transforms from confusion to clarity, from silent endurance to informed strength.
As we continue this journey across women’s health, the next we will explore a dimension that is inseparable from hormonal wellbeing. The future of women’s health is not built by treating systems in isolation instead it is built by understanding the whole girl, the whole woman, and the whole life journey. Let’s see how social expectations, digital culture, academic stress, and biological changes converge to shape the emotional health of adolescent girls.
- World Health Organization. Polycystic Ovary Syndrome (PCOS).
https://www.who.int/news-room/fact-sheets/detail/polycystic-ovary-syndrome - Office on Women’s Health. Polycystic Ovary Syndrome.
https://www.womenshealth.gov/a-z-topics/polycystic-ovary-syndrome - UNICEF. Adolescent Health Overview.
https://www.unicef.org/adolescence